Justin Smarsh, a 42-year-old former coal miner from Cherry Tree, Pennsylvania, remembers a time when the Appalachian Plateau offered a life of rugged outdoor activity. He once spent his weekends kayaking the winding rivers near his home and teaching his two sons how to hunt in the dense woods northeast of Pittsburgh. Today, those memories feel like a different lifetime. Smarsh describes a sensation of being "suffocated just walking." A simple task like bending down to tie his shoes leaves him gasping for air, and a persistent, dry cough has become the soundtrack of his daily life.
Smarsh is a third-generation miner, having followed his father and grandfather into the pits shortly after high school because it was, and remains, the highest-paying job in his rural county. However, the cost of that paycheck has been his health. He has been diagnosed with progressive massive fibrosis (PMF), the most advanced and lethal stage of coal workers’ pneumoconiosis, commonly known as black lung. There is no cure. His medical regimen consists of "piles of meds" intended to slow the inevitable, but his physicians have delivered a grim prognosis: he is unlikely to see his 50th birthday.
The Silent Epidemic in Modern Mining
The tragedy of Justin Smarsh is not an isolated incident. Despite a public perception that coal mining is a fading industry of the past, medical professionals in Appalachia are witnessing a terrifying resurgence of the disease. Deanna Istik, CEO of Lungs at Work, a specialized clinic in Washington County, Pennsylvania, notes that her facility is seeing more black lung diagnoses than ever before.

The nature of the disease has changed, becoming more aggressive and striking younger workers. Historically, black lung was the result of decades of inhaling coal dust. However, modern miners are being exposed to something far more toxic: crystalline silica. As the massive, easily accessible coal seams of Appalachia have been exhausted over the last century, mining companies have turned to thinner seams. To reach these deposits, miners must cut through significant amounts of sandstone and quartz. When these rocks are pulverized by heavy machinery, they release microscopic particles of silica.
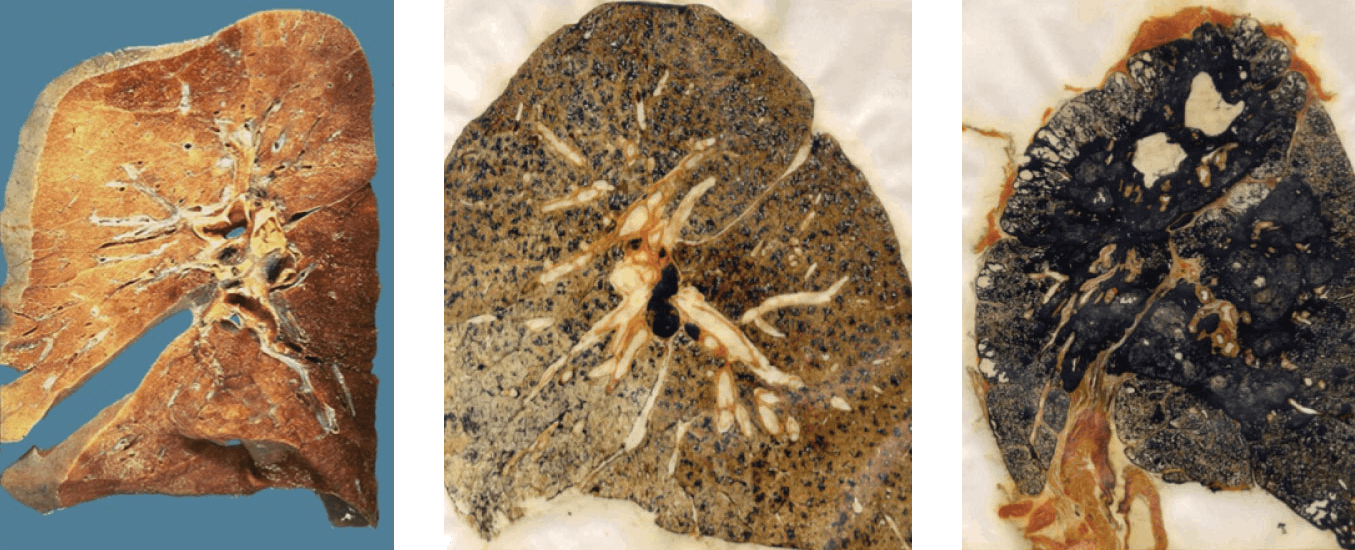
When inhaled, these silica particles act like tiny shards of glass, embedding themselves deep in the lung tissue. This triggers an intense immune response where the body attempts to wall off the foreign particles, leading to severe inflammation, scarring, and the formation of blackened, fibrotic masses. This accelerated form of the disease can disable a worker in less than a decade, compared to the 30 or 40 years it took for previous generations to develop symptoms.
A Chronology of Regulation and Resurgence
To understand the current crisis, one must look at the history of mine safety in the United States. The struggle for breathable air in the mines has been a decades-long battle between labor advocates, government regulators, and industrial interests.
- 1968-1969: Following the Farmington Mine disaster in West Virginia, which killed 78 miners, a wave of strikes forced Congress to pass the 1969 Federal Coal Mine Health and Safety Act. This landmark legislation established the first federal standards for coal dust and created a benefits program for afflicted miners.
- 1970s-1990s: For a period, the regulations worked. Increased inspections and better ventilation systems led to a dramatic decline in black lung cases. By the late 1990s, the disease was considered nearly eradicated in many regions.
- 2000-2010: As mining technology improved and thin-seam mining became more common, health experts began to notice a "hotspot" of new cases in Central Appalachia.
- 2013-2017: Researchers from the National Institute for Occupational Safety and Health (NIOSH) identified hundreds of cases of PMF at clinics in Virginia. This led NIOSH to officially declare a renewed epidemic.
- 2024: After years of lobbying and scientific review, the Mine Safety and Health Administration (MSHA) announced a final rule to lower the permissible exposure limit for silica dust from 100 micrograms per cubic meter to 50 micrograms, matching standards in other industries.
- 2025-2026: Implementation of the new silica rule faced immediate legal challenges and administrative delays. In April 2025, an emergency stay was granted by the 8th U.S. Circuit Court of Appeals. By early 2026, MSHA announced the delay would continue "indefinitely" pending further judicial and administrative review.
Statistical Realities and Economic Pressures
The resurgence of black lung is occurring against a backdrop of complex economic shifts. While coal production in the U.S. has fallen by more than 50 percent since its peak in 2008—dropping from 1,170 million tons to approximately 578 million tons in 2023—the industry remains a vital economic pillar for certain regions. In Pennsylvania alone, coal mining generates roughly $2.2 billion in economic output and supports over 5,000 direct jobs.

Nationwide, approximately 40,000 workers remain in the coal industry. For these workers, the health risks are stark. NIOSH estimates that one in ten miners who have worked underground for at least 25 years now has black lung. Among those in the Appalachian regions of Virginia, West Virginia, and Pennsylvania, the rate is even higher. Furthermore, mortality data shows that after declining for two decades, black-lung-associated deaths began to rise again between 2020 and 2023.
The tragedy is compounded by the fact that the disease is often underreported. Many miners, fearful of losing their high-paying jobs or facing retribution from employers, avoid medical screenings until their symptoms are too severe to ignore. "There’s always going to be that fear of retribution," says Istik. By the time a miner like Smarsh seeks help, the damage is usually irreversible.
Policy Shifts and Regulatory Rolbacks
The recent uptick in diagnoses coincides with a political push to revitalize the coal industry. Under the current administration, coal has been reaffirmed as essential to national security, a move that directs billions of dollars in federal funding toward coal projects and infrastructure. In late 2023, the U.S. Department of Energy announced a $625 million investment in coal-related technology.
However, advocates argue that this push for production has come at the expense of safety. MSHA, the agency responsible for protecting miners, has seen significant budget and staffing cuts over the last decade. Enforcement staff has been cut nearly in half, and recent federal "buyout" programs have led to a loss of veteran inspectors with decades of experience.
The delay of the silica rule is the most contentious point of conflict. The mining industry, represented by groups like the National Mining Association (NMA) and the National Stone, Sand & Gravel Association, argues that the 50-microgram standard is technically difficult to achieve through ventilation alone. They have lobbied for the right to use respirators as a primary means of compliance.
Labor advocates and health experts, however, reject this proposal. Erin Bates, communications director for the United Mine Workers of America (UMWA), emphasizes that respirators are a "last line of defense" and are often impractical in the hot, cramped, and dusty environment of a mine. "It should not be the coal miner’s responsibility not to get black lung," Bates said. "It is the company that must ensure a safe work environment."
Implications for the Future of Appalachia
The indefinite delay of silica protections has left mining communities in a state of uncertainty and grief. For families like the Smarshes, the impact is generational. Justin Smarsh’s 19-year-old son has expressed interest in entering the mines, a prospect that fills his father with dread. Smarsh warns his son that the "good coal" is gone, replaced by toxic rock and silica.
The broader implications for the Appalachian region are profound. As more young miners are diagnosed with disabling lung diseases, the long-term healthcare costs will fall on local systems and federal benefit programs. The Black Lung Disability Trust Fund, which provides compensation to miners whose employers have gone bankrupt, has frequently faced insolvency, necessitating federal intervention.

Furthermore, the surge in PMF cases has led to an increased demand for lung transplants, a high-risk and prohibitively expensive procedure that offers only a marginal increase in life expectancy for many patients.
Conclusion: A Moral and Medical Crisis
The story of black lung in the 21st century is a narrative of technological progress clashing with human vulnerability. While mining machinery has become more efficient at extracting coal from deep within the earth, the protections for the humans operating that machinery have not kept pace with the changing geology of the mines.
For experts like Rebecca Shelton of the Appalachian Citizens’ Law Center, the current regulatory limbo is a failure of government oversight. "If the administration actually cared about protecting coal miners from black lung, we’d have a strong silica rule in place right now," Shelton stated. Instead, the legal and administrative delays mean that another generation of miners will continue to breathe air that is effectively a death sentence.
As for Justin Smarsh, he remains a vocal witness to the costs of the industry. His message to his son and to his community is one of caution and disillusionment. He believes the companies prioritize "black gold" over human life. "They say they care about miners," Smarsh said, "but you go underground, you’re taking the risk, for you to get nothing but sick, and to fill their pockets full."







Leave a Reply