A Florida grand jury has delivered a scathing indictment against surgeon Thomas Shaknovsky, charging him with second-degree manslaughter for the 2024 death of 70-year-old William Bryan of Alabama. The tragic incident, which unfolded during what was intended to be a routine splenectomy, has cast a grim spotlight on surgical accountability and patient safety protocols within the medical community. Bryan’s death, resulting from a procedure described by state investigators as horrifyingly botched, involved the severance of his body’s largest vein and the removal of his healthy liver instead of his spleen.
Indictment Details and Legal Ramifications
The indictment by the Florida grand jury marks a significant escalation in the legal repercussions faced by Dr. Shaknovsky. Second-degree manslaughter in Florida carries a potential sentence of up to 15 years in prison upon conviction. This criminal charge stems from an exhaustive investigation conducted by the Walton County Sheriff’s Office, working in close coordination with the Office of the State Attorney First Judicial Circuit, as well as various state and medical authorities. The decision by the grand jury to indict underscores the severity with which the authorities view the events leading to Mr. Bryan’s demise.
Walton County Sheriff Michael Adkinson, in announcing Shaknovsky’s indictment, affirmed the commitment of the legal system: "The Grand Jury has spoken, and our responsibility is to ensure the charges are carried out through the proper legal process. Our thoughts remain with the victim’s family and their unspeakable loss." Dr. Shaknovsky was arrested on a Monday morning and subsequently released on bond, awaiting the progression of his trial. The legal proceedings are expected to be complex, delving deep into the minutiae of medical practice, surgical standards, and the specific actions of the surgeon during the fatal procedure.
The Patient’s Ordeal: From Vacation to Tragedy
William Bryan, a 70-year-old resident of Alabama, had traveled to Florida with his wife for a vacation when his health took an unexpected turn. He developed severe pain in his upper left abdomen, prompting a visit to the emergency department of a hospital in Miramar Beach. Dr. Shaknovsky, serving as the on-call general surgeon, assessed Mr. Bryan. Initial imaging studies suggested a potentially enlarged spleen and the presence of blood in the peritoneal membrane lining the abdominal cavity, though no active hemorrhage was observed at that time.
Dr. Shaknovsky advised Mr. Bryan that a splenectomy – the surgical removal of the spleen – was necessary. However, Mr. Bryan initially expressed reluctance, indicating a preference to return to Alabama for treatment at a facility offering a higher level of specialized care. According to a lawsuit subsequently filed by his widow, Dr. Shaknovsky allegedly exerted considerable pressure on Mr. Bryan over the ensuing days, ultimately convincing him to undergo the surgery in Florida. This detail highlights a critical aspect of patient autonomy and informed consent, particularly when a patient expresses reservations or seeks alternative care options. The decision to proceed with surgery under such circumstances, especially when a patient’s condition might not be immediately life-threatening, often involves careful consideration of risks, benefits, and alternatives.
A Surgical Nightmare Unfolds: The Botched Procedure
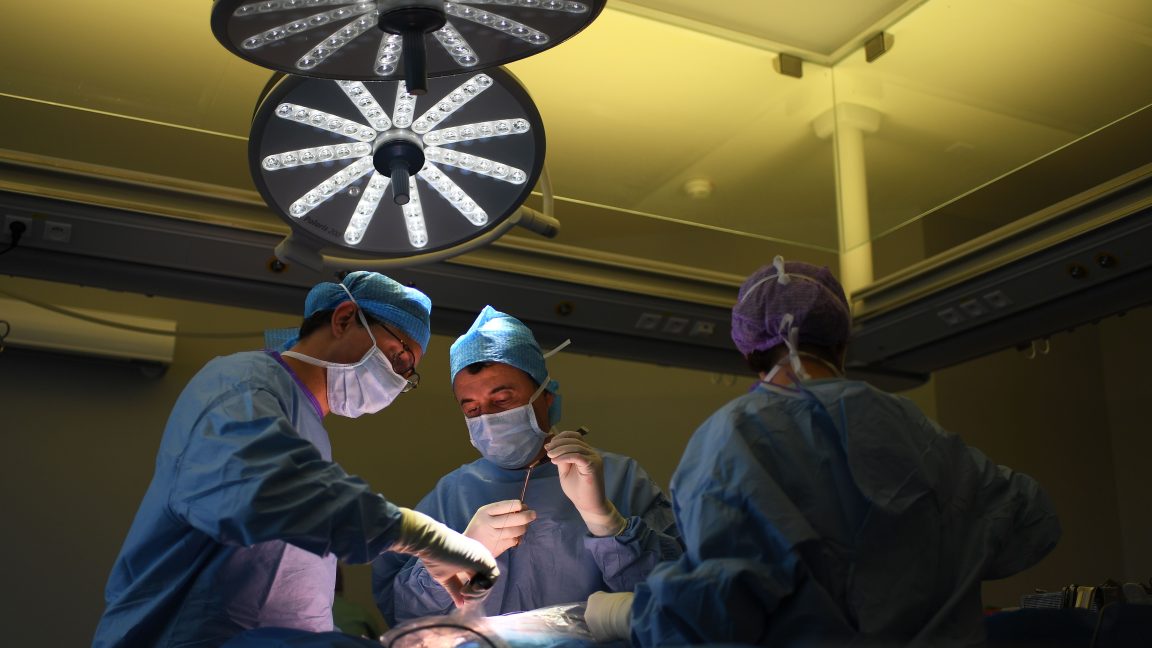
The operation, initially scheduled for 4 p.m., quickly deviated from standard protocols. Dr. Shaknovsky arrived at the hospital an hour late, and Mr. Bryan was brought into the operating room (OR) around 5:20 p.m., a time when only a skeleton crew was reportedly available. This staffing detail raises questions about resource allocation and the hospital’s operational readiness for complex procedures.
The initial plan for a minimally invasive (laparoscopic) procedure was swiftly abandoned. Dr. Shaknovsky, after commencing the operation, encountered a distended colon that obstructed his view, prompting an immediate conversion to an open abdominal surgery. While converting from laparoscopic to open surgery is not uncommon in itself, the subsequent events were catastrophic. OR staff members, interviewed by health department investigators, recounted how Mr. Bryan’s colon "burst out" when Dr. Shaknovsky made the incision, requiring them to rush in to reposition the organ and suction accumulating blood.
In a chilling moment, Dr. Shaknovsky reportedly identified a blood vessel he intended to sever. He noted to the assisting staff that he could feel it pulsing under his fingers, allegedly remarking, "That’s scary." This comment, recorded in investigative reports, suggests a potential misidentification or at least a moment of uncertainty regarding the anatomical structure being targeted. Despite this apparent apprehension, Dr. Shaknovsky proceeded. He grabbed a surgical stapler, positioned it around the vessel, and fired.
The consequences were immediate and devastating. Mr. Bryan began hemorrhaging severely and rapidly went into cardiac arrest. OR staff described a "significant amount of blood" pouring out, triggering an emergency blood transfusion protocol. A "code" was called, and CPR commenced. Alarmingly, Dr. Shaknovsky reportedly continued to work within Mr. Bryan’s abdomen, which was by then filled with a pooling mass of blood. Despite the lack of clear visibility, he did not request a clamp or cauterizer – standard instruments for controlling bleeding. Instead, investigators found, Dr. Shaknovsky "blindly fired another staple" into Mr. Bryan’s abdomen and continued his efforts.
The Unbelievable Discovery: A Liver, Not a Spleen
After prolonged and ultimately futile attempts by the medical staff to resuscitate Mr. Bryan, he was pronounced dead. In the aftermath, Dr. Shaknovsky extracted an organ, which he identified as Mr. Bryan’s spleen, and placed it on a table. The reaction of the OR staff, however, was one of profound shock and disbelief. They reportedly looked at the organ, which was "readily identifiable" as a liver, causing one staff member to feel "sick to their stomach."
The anatomical discrepancies between the organ removed and the intended target were stark and undeniable. The liver Dr. Shaknovsky had extracted weighed over 2,100 grams and measured approximately 23 by 19 by 11 centimeters. In contrast, an enlarged spleen, such as Mr. Bryan’s was thought to be, typically weighs at most 500 grams and measures up to 20 centimeters in length. Beyond size, livers and spleens are anatomically distinct organs, differing significantly in color, texture, and consistency. Furthermore, the liver is situated on the right side of the abdomen, while the spleen is located on the left – the side Mr. Bryan had indicated was the source of his pain.
Despite these glaring differences and the evident distress of his staff, Dr. Shaknovsky reportedly insisted that the removed organ be labeled as a spleen. Disturbingly, he returned to the operating room three times that evening, attempting to persuade staff members that it was indeed a spleen. The subsequent pathology report, a crucial piece of evidence, unequivocally described the so-called spleen as "a grossly identifiable 2,106 g liver." An autopsy further confirmed the horrific extent of the error: Mr. Bryan’s spleen was found to be completely intact, his liver was missing, and his inferior vena cava – the largest vein in the body, responsible for returning deoxygenated blood from the lower body to the heart through the liver – had been severed. The immediate and complete severance of such a critical vessel would have led to rapid, irreversible exsanguination and cardiac arrest, as observed during the surgery.
A Disturbing Pattern: Previous Misidentifications

As investigators delved into the ghastly details of Mr. Bryan’s death, a deeply troubling revelation emerged: this was not Dr. Shaknovsky’s first instance of removing the wrong organ. In 2023, just a year prior to Mr. Bryan’s death, Dr. Shaknovsky had mistakenly removed a portion of a patient’s pancreas when his stated intention was to remove the adrenal gland. In his post-operative report for that incident, he bizarrely claimed that the adrenal gland had "migrated," an anatomical impossibility that further casts doubt on his diagnostic judgment and surgical precision.
This pattern of egregious surgical errors raises profound questions about Dr. Shaknovsky’s competence, adherence to surgical safety protocols, and the oversight mechanisms in place at the facilities where he practiced. The repeated misidentification of major organs, particularly those with distinct anatomical features and locations, is an anomaly in modern surgical practice, which heavily relies on meticulous pre-operative planning, intra-operative verification, and adherence to established safety checklists.
Official Responses and Broader Implications for Patient Safety
The immediate aftermath of Mr. Bryan’s death saw swift action from regulatory bodies. In September 2024, Florida State Surgeon General Joseph Ladapo ordered an emergency suspension of Dr. Shaknovsky’s medical license. An emergency suspension is a severe administrative action typically taken when a medical professional poses an immediate and serious danger to the public health, safety, or welfare. The detailed findings of the state health department’s investigation provided the comprehensive basis for this decisive action, effectively preventing Dr. Shaknovsky from practicing medicine.
This case, while extreme, highlights critical issues within the broader medical system. Surgical errors, though rare, are a persistent concern in healthcare. To combat such incidents, organizations like the World Health Organization (WHO) advocate for universal adoption of the Surgical Safety Checklist, which includes crucial "time-out" procedures. A "time-out" is a mandatory pause before the start of any surgical procedure, during which the entire surgical team confirms the patient’s identity, the correct surgical site, and the procedure to be performed. This protocol is designed specifically to prevent wrong-site, wrong-procedure, and wrong-patient errors. The detailed account of Mr. Bryan’s surgery suggests a profound failure to adhere to, or an inability to properly execute, such fundamental safety measures.
The civil lawsuit filed by Mr. Bryan’s widow remains pending, seeking accountability and compensation for their immeasurable loss. Her powerful statement to NBC News underscores the family’s motivation: "He would want his death to prevent someone else from being hurt, which is what I think the criminal charges being brought will do. If we had to suffer through this and he had to die, then at least no one else will be hurt by this man now." Her words reflect a universal desire for justice and for systemic improvements that protect future patients from similar tragedies.
This incident is likely to prompt a review of surgical protocols, credentialing processes, and oversight mechanisms not only in Florida but potentially across the nation. The medical community faces the challenge of reassuring public trust while rigorously enforcing standards of care and accountability for practitioners whose actions fall catastrophically short. The legal proceedings against Dr. Shaknovsky will undoubtedly be closely watched, as they represent a rare instance of criminal charges being brought against a surgeon for actions taken in the operating room. The outcome will have significant implications for the intersection of medical practice, patient safety, and legal accountability. The tragic death of William Bryan serves as a somber reminder of the profound responsibility entrusted to surgeons and the devastating consequences when that trust is breached.







Leave a Reply